The immune system has antibodies, the cardiovascular system has red blood cells, and the nervous system has electrical impulses.
Ever wonder what your body’s endocannabinoid system runs on?
Or maybe you’re just wondering what this endocannabinoid system (ECS) is in the first place. Either way, let’s start with the basics before addressing the endogenous cannabinoids that make your ECS tick. Here’s an outline:
What Is the Endocannabinoid System?
The endocannabinoid system, or ECS for short, is a special chemical signaling system that all vertebrates have.
Think of it like your body’s natural version of the internet. In today’s world, businesses and economies would crash without the communication the world wide web has facilitated. Without our endocannabinoid systems, the impact on our biology would be much the same.
The endocannabinoid system has several different parts, and its presence can be seen throughout virtually the entire body: in the brain, in every important organ and even in muscle tissue and mitochondria. Even people who’ve never taken CBD, THC, or any other cannabis/hemp-related substance have been producing endocannabinoids their whole lives.
In general, the more complex a life form is, the more advanced its endocannabinoid system—a powerful testament to how critical this system is to holding all the elements that comprise a living system together.
When Was the Endocannabinoid System Discovered?
For something as significant as it is, the endocannabinoid system stayed under science’s radar for a surprisingly long time prior to its discovery in the 90s.
Actually, maybe not so surprisingly. Just like we often take for granted the air around us and the oxygen we breath, the ECS is ubiquitous enough that no one really knew what specific markers to look for.
The 1960’s Discoveries
The cannabis plant was actually what first gave researchers some clues. In the 1960s, an Israeli researcher named Raphael Mechoulam started doing his own research. Trained in the field of natural products chemistry, Mechoulam knew there must be more to cannabis than meets the eye. While the active ingredients of many pharmaceuticals had been elucidated more than 100 years prior, Mechoulam noted that “the chemistry of cannabis was not well known.”
Together with other researchers at the Hebrew University of Jerusalem, and powered by cutting-edge nuclear magnetic resonance technology, Mechoulam’s team put cannabis under the literal microscope (or spectroscope, actually). In 1963 the chemical makeup, or stereochemistry, of CBD was fully identified. THC’s identification came next, in 1964.
Even after these breakthroughs, however, scientists didn’t have any idea how CBD and THC actually worked. What made THC so psychotropic? And why was CBD so decidedly non-psychotropic . . . despite sharing such a similar chemical structure?
Initial research brought about more questions than answers. Why? Because the endocannabinoid system—not to mention its hard-working endocannabinoids—hadn’t yet been discovered.
“There was no conception [of endocannabinoids],” Mechoulam, now in his late 80’s, explained at a 2017 medical conference. “The mechanism of THC action was not known. People thought it had a general effect. . . . [T]he theory was that THC solubilizes in the cell membrane or something of that sort.”
“It turns out that was wrong.”
Research Progresses
A breakthrough finally came in 1990, when Mechoulam’s team made another pivotal discovery. What did they find? A G-protein-coupled-receptor, the most common class of receptors in the brain, that could be directly activated by THC. They called it cannabinoid receptor type one, or CB-1.
The implications of this discovery were huge. To the scientifically trained mind, it meant more was out there. Something else had to be activating these unique receptors; it couldn’t just be plants. Mechoulam relays some more of his thoughts, again from 2017’s medical congress:
“Now, receptors don’t exist because there’s a plant out there; receptors exist because we, through compounds made in our body, activate them. So we went looking for the endogenous compounds that activate the cannabinoid receptors. We managed to identify a compound, in 1992, and we called it anandamide.”
Anandamide: a clever combo of the Sanskrit term for bliss or “supreme joy” and a scientific suffix, put together to mean “the bliss molecule.” With anandamide’s discovery, science finally had a firm grasp on the endocannabinoid system and its function.
The Endocannabinoid System’s Surprising Role
All this review of the research leads us to one thing: the endocannabinoid system’s real role. What does the system do?
Beyond what’s already been mentioned, the ECS’s primary function is simple. It helps us adapt to and overcome stress by helping our bodies communicate . . . with every part of themselves. The endocannabinoid system may not be exactly like our internal internet, but it’s definitely a body-wide-web. It promotes inner homeostasis in a way unmatched by anything else.
How? As it turns out, the endocannabinoid system has three main parts, and all three of them play a vital role in reducing stress and promoting balance: there’s endocannabinoid receptors, endocannabinoids, and the enzymes that break the latter down.
Endocannabinoids
Endocannabinoids are the endocannabinoid system’s favorite cellular messengers. They’re small, short-lived molecules made of the same healthy fats that comprise our cells’ lipid membranes. In fact, endocannabinoids are literally ‘pushed’ out of this membrane when stress dictates. The two most common endocannabinoids are anandamide and 2-AG.
And although these are the most common, there are many more. Dr. Bob Melamede has explained that “numerous other related molecules also appear to [have] related endocannabinoid-like activity.” According to him, these substances include
- N-arachidonoylglycine
- Stearoyl-ethanolamide
- N-arachidonoyldopamine
- Homo-g-linolenylethanolamide
- 7,10,13,16-Docosatetraenylethanolamid virodhamine
- Noladin ether
Tongue twisters aside, just know that the endocannabinoid system has more than a few messenger molecules at its disposal. And while the most commonly-known eCB’s are made of omega-6 fatty acids, other researchers have discovered a new class of endocannabinoids made of omega-3’s. No wonder both types of fats are so essential!
Endocannabinoid Receptors
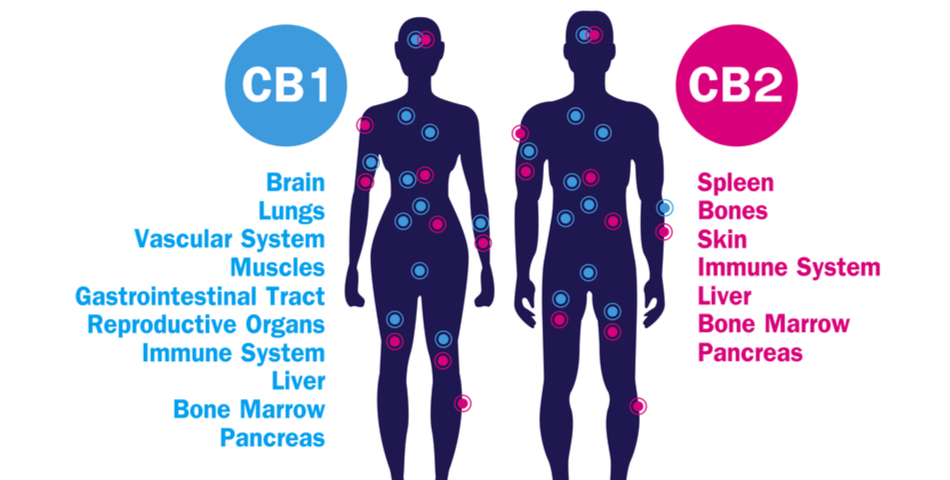
As described in the research overview a little earlier, the endocannabinoid system’s receptors were the first thing to be discovered. There are two primary types of endocannabinoid receptors in the brain, appropriately titled CB1 and CB2. CB1 tends to receive ‘messages’ from THC and analogous endocannabinoids, while CB2 receives messages from CBD and endocannabinoids like it
Amazingly enough, CB1 and CB2 are the most prevalent type of GPCR’s (G-protein-coupled-receptors) in the human brain. Just think of what that means: they’re more highly concentrated than the receptors that control GABA or serotonin or dopamine. And they’re there for a reason, the primary reason being to normalize overall brain function by working with endocannabinoids. As a practical example of this type of normalization, look no further than what happens when CBD and other cannabinoids are given to children with epilepsy: brain function often normalizes. Indeed, thousands of parents have reported that their children’s seizures virtually ceased.
But endocannabinoid receptors can also be found outside the brain. The entire digestive tract is full of them; poor endocannabinoid health there, in fact, has been correlated with inflammatory conditions like IBS and leaky gut. Muscle cells strongly express CB2, an expression that may be increased by healthy living and exercise. Even our mitochondria have endocannabinoid receptors built into their membranes. The message from all this is clear: our bodies are uniquely suited to receive crucial input from cannabinoids of all sorts.
Endocannabinoid Enzymes
Last, but not least, is the third facet of the endocannabinoid system: its enzymes. There are two major types of enzymes. Some synthesize endocannabinoids from their fatty-acid precursors, while others break them down.
Let’s take a look at the breakdown enzymes first. The life of any individual endocannabinoid is short-lived, and it’s that way for a reason: eCB’s are meant to respond to stress in real time, not stick around when they’re not needed. Breakdown enzymes serve to ‘recycle’ used endocannabinoids as soon as they’ve sent their messages.
Synthesizing enzymes have the opposite effect. They help stressed cells form endocannabinoids quickly and efficiently, especially in times of stress. These enzymes initiate complex chemical reactions that turn omega-6 fats into more specialized molecules. It’s basically cellular alchemy!
How the ECS Regulates Your Brain
We’ve already talked a little about how many endocannabinoids and receptors are present in the brain. But what do they actually do there, and how do they maintain this homeostasis you’ve heard mentioned?
Nerd alert: it’s a little complex. Endocannabinoids help regulate brain function through something called retrograde signaling. While the brain sends most of its important signals by essentially pushing them along with electrical impulses, eCB’s operate independently from all this. They’re controlled by pressure gradients that allow them to travel backward across synapses, and they send messages to the specific areas where most other messages—those involving GABA, serotonin, dopamine, et cetera—are being sent from.
Basically, the endocannabinoid system helps regulate one’s brain function because it’s full of built-in feedback loops. The endocannabinoids complete these loops and help normalize all sorts of neurotransmitter-based functions.
Clinical Endocannabinoid Deficiency Syndrome
Though the endocannabinoid system is amazing, it’s not immune to developing imbalances of its own. In fact, the system is so crucial that any imbalance in it can cause some pretty serious problems. Among the suspected side effects are diseases like fibromyalgia, chronic migraines, epilepsy, and more. Welcome to the strange world of endocannabinoid deficiency syndrome.
The idea that endocannabinoid levels could manifest as specific disease states was first introduced by Dr. Ethan Russo, botanical expert and former advisor for GW pharmaceuticals (yes, the same company that would later roll out Epidiolex).
Dr. Russo’s theory reached the mainstream around 2004, when he published an appropriately-titled study, “Clinical endocannabinoid deficiency (CECD): can this concept explain therapeutic benefits of cannabis in migraine, fibromyalgia, irritable bowel syndrome and other treatment-resistant conditions?”
In this research article he made a fairly convincing case that many pain-based conditions are actually caused by chronically low endocannabinoid levels. Considering that endocannabinoids like anandamide are known to reduce pain, Russo’s theory made intuitive sense
Speaking to Project CBD in 2016, Russo explained his reasoning
“[Things like] migraines, irritable bowel syndrome, and fibromyalgia [ . . . ] they’re all hyper-algesic syndromes, meaning that there seems to be pain out of proportion to what should be going on.” The endocannabinoid system is so influential on our perception, the thinking goes, that any imbalance in it would lead us to perceive things—in this case, aches and pains—that we don’t actually need to.
How CBD Could Help Your Inner Balance
How to deal with these problems? Russo and our team here at Green Maiden agree: supplement with phytocannabinoids! Just as vitamin C might raise immunity by substituting for endogenous antioxidants, CBD might be able to promote balance by encouraging the body to make more of its own cannabinoids.
We’ve also been inspired by Russo’s advocacy for whole plant medicine and the entourage effect. There’s more to hemp than meets the eye, and there’s actually more to promoting endocannabinoid health than supplementing with one or two molecules.
To sum up, from a thermodynamic perspective, the world is a pretty demanding place—although you probably didn’t need a scientific explanation to tell you that stress-reduction is important! And by helping us deal with stress, endocannabinoids help us thrive. If you haven’t found your ‘thrive’ yet, don’t worry—plant cannabinoids like CBD may be able to help.
Green Maiden




